Addictions
New lawsuit challenges Ontario’s decision to prohibit safe consumption services

Kensington Market Overdose Prevention Site in Toronto, Dec. 18, 2024. [Photo credit: Alexandra Keeler]
Critics says Ontario’s plan to replace supervised consumption sites with HART Hubs will exacerbate harms to drug addicts and strain the health-care system
The operator of a Toronto overdose prevention site is challenging Ontario’s decision to prohibit 10 supervised consumption sites from offering their services.
In December, Neighbourhood Group Community Services and two individuals launched a constitutional challenge to Ontario legislation that imposes 200-metre buffer zones between supervised consumption sites and schools and daycares. The Neighbourhood Group will be forced to close its site in Toronto’s Kensington Market as a result.
In its court challenge, the organization is arguing site closures discriminate against individuals with “substance use disabilities” and increase drug users’ risk of death and disease.
The challenge is the latest sign of growing opposition to Ontario’s decision to either shutter supervised consumption sites or transition them into Homelessness and Addiction Recovery Treatment (HART) Hubs. The hubs will offer drug users a range of primary care and housing solutions, but not supervised consumption, needle exchanges or the “safe supply” of prescription drugs.
Critics say the decision to suspend supervised consumption services will harm drug users and the health-care system.
“We’re very happy that the HART Hubs are being funded,” said Bill Sinclair, CEO of Neighbourhood Group Community Services. “They’re a great asset to the community.”
“[But] we want HART Hubs and we want supervised consumption sites.”
Our content is always free.
Subscribe to get BTN’s latest news and analysis, or donate to our journalism fund.
‘Come under fire’
On Thursday, the Ontario government announced that nine of the 10 supervised consumption sites located near centres with children would transition into HART Hubs. The Neighbourhood Group’s site is the only one not offered the opportunity to transition, because it is not provincially funded.
Laila Bellony, a harm reduction manager at a supervised consumption site at the Parkdale Queen West Community Health Centre in Toronto, says she is worried that drug users may avoid using HART Hubs altogether if they do not facilitate the use of drugs under the supervision of trained staff.
Data show this oversight can prevent deaths by facilitating immediate intervention in the event of an overdose.
Bellony is also concerned the site closures will increase the strain on other health-care services. She predicts longer wait times and bed shortages in hospital emergency rooms, as well as increased paramedic response times.
“I think the next thing that will happen is the medical or health-care system is going to come under fire for being sub-par. But it’s really all starting here from this decision,” she said.
She questions how the HART Hubs will meet demand for detox and recovery services or housing solutions.
Parkdale Queen West Community Health Centre and its sister site, the Queen West Site, serve hundreds of clients, Bellony says. By contrast, Ontario’s HART Hub rollout plan indicates all 19 hubs will together provide 375 new housing units across the province.
“The HART Hub model is not a horrible model,” said Bellony. “It’s the way that it’s being implemented that’s ill-informed.”
In a response to requests for comment, a media spokesperson for the Ontario Ministry of Health directed Canadian Affairs to its August news release. That release lists proposals for increased safety measures at remaining sites, and a link to a HART Hub “client journey.”
On Dec. 3, the Auditor General of Ontario, Shelley Spence, released a report criticizing the health ministry’s “outdated” opioid strategy, noting it has not been updated since 2016.
National data show a 6.7 per cent drop in opioid deaths in early 2024. But experts caution it is too soon to call it a lasting trend. Opioid toxicity deaths in 2023 were up 205 per cent from 2016.
“We concluded that the Ministry does not have effective processes in place to meet the challenging and changing nature of the opioid crisis in Ontario,” the auditor general’s report says.
“The Ministry did not … provide a thorough, evidence-based business case analysis for the 2024 new model … [HART Hubs] to ensure that they are responsive to the needs of Ontarians.”
 |
Parkdale Queen West Community Health Centre’s Queen West Site in Toronto, Dec. 18, 2024. [Photo credit: Alexandra Keeler]
‘Ill-informed’
Ontario has cited crime and public safety concerns as reasons for blocking supervised consumption sites near centres with children from offering their services.
“In Toronto, reports of assault in 2023 are 113 per cent higher and robbery is 97 per cent higher in neighbourhoods near these sites compared to the rest of the city,” Ontario Health Minister Sylvia Jones’ office said in an Aug. 20 press release.
The province has also cited concerns about prescription drugs dispensed through safer supply programs being diverted to the black market.
Police chiefs and sergeants in the Ontario cities of London and Ottawa have confirmed safer supply diversion is occurring in their municipalities.
“We are seeing significant increases in the availability of the diverted Dilaudid eight-milligram tablets, which are often prescribed as part of the safe supply initiatives,” London Police Chief Thai Truong said at a Nov. 26 parliamentary committee meeting examining the effect of the opioid epidemic and strategies to address it.
But Bellony disputes the claim that neighbourhoods with supervised consumption sites experience higher crime rates.
“Some of the things that [the ministry is] saying in terms of crime being up in neighborhoods with safe consumption sites — that’s not necessarily true,” she said.
In response to requests for information about the city’s crime rates, Nadine Ramadan, a senior communications advisor for the Toronto Police Service, directed Canadian Affairs to the service’s crime rate portal.
The portal shows assaults, break-and-enters and robberies in the West Queen West neighborhood have remained relatively stable since the Queen West supervised consumption site opened in 2018.
In contrast, crime rates are higher in some nearby neighbourhoods without supervised consumption sites, such as The Junction.
“While I can’t speak to perceptions about a rise in crime specifically around supervised consumption sites, I can tell you that violent crime is increasing across the GTA,” Ramadan told Canadian Affairs. She referred questions about Jones’ statements about crime data to the health minister’s office.
Jones’ office did not respond to multiple follow-up inquiries.
Mixed feelings
In July, Canadian Affairs reported that business owners in the West Queen West neighbourhood were grappling with a surge in drug-related crime.
Rob Sysak, executive director of the West Queen West Business Improvement Association, says there are mixed feelings about their neighbourhood’s site ceasing to offer safe consumption services.
“I’m not saying [the closure] is a positive or negative decision, because we won’t know until after a while,” said Sysak, whose association works to promote business in the area.
Sysak says he has heard concerns from business owners that needles previously used by individuals at the site may now end up on the street.
Bellony supports the concept of HART Hubs offering addiction and support services. But she says she finds the province’s plan for the hubs to be unclear and unrealistic.
“It seems very much like they kind of skipped forward to the ideal situation at the end,” she said. “But all the steps that it takes to get there … are unaddressed.”
This article was produced through the Breaking Needles Fellowship Program, which provided a grant to Canadian Affairs, a digital media outlet, to fund journalism exploring addiction and crime in Canada. Articles produced through the Fellowship are co-published by Break The Needle and Canadian Affairs.
Our content is always free – but if you want to help us commission more high-quality journalism, consider getting a voluntary paid subscription.
Addictions
Addiction experts demand witnessed dosing guidelines after pharmacy scam exposed

By Alexandra Keeler
The move follows explosive revelations that more than 60 B.C. pharmacies were allegedly participating in a scheme to overbill the government under its safer supply program. The scheme involved pharmacies incentivizing clients to fill prescriptions they did not require by offering them cash or rewards. Some of those clients then sold the drugs on the black market.
An addiction medicine advocacy group is urging B.C. to promptly issue new guidelines for witnessed dosing of drugs dispensed under the province’s controversial safer supply program.
In a March 24 letter to B.C.’s health minister, Addiction Medicine Canada criticized the BC Centre on Substance Use for dragging its feet on delivering the guidelines and downplaying the harms of prescription opioids.
The centre, a government-funded research hub, was tasked by the B.C. government with developing the guidelines after B.C. pledged in February to return to witnessed dosing. The government’s promise followed revelations that many B.C. pharmacies were exploiting rules permitting patients to take safer supply opioids home with them, leading to abuse of the program.
“I think this is just a delay,” said Dr. Jenny Melamed, a Surrey-based family physician and addiction specialist who signed the Addiction Medicine Canada letter. But she urged the centre to act promptly to release new guidelines.
“We’re doing harm and we cannot just leave people where they are.”
Addiction Medicine Canada’s letter also includes recommendations for moving clients off addictive opioids altogether.
“We should go back to evidence-based medicine, where we have medications that work for people in addiction,” said Melamed.
‘Best for patients’
On Feb. 19, the B.C. government said it would return to a witnessed dosing model. This model — which had been in place prior to the pandemic — will require safer supply participants to take prescribed opioids under the supervision of health-care professionals.
The move follows explosive revelations that more than 60 B.C. pharmacies were allegedly participating in a scheme to overbill the government under its safer supply program. The scheme involved pharmacies incentivizing clients to fill prescriptions they did not require by offering them cash or rewards. Some of those clients then sold the drugs on the black market.
In its Feb. 19 announcement, the province said new participants in the safer supply program would immediately be subject to the witnessed dosing requirement. For existing clients of the program, new guidelines would be forthcoming.
“The Ministry will work with the BC Centre on Substance Use to rapidly develop clinical guidelines to support prescribers that also takes into account what’s best for patients and their safety,” Kendra Wong, a spokesperson for B.C.’s health ministry, told Canadian Affairs in an emailed statement on Feb. 27.
More than a month later, addiction specialists are still waiting.
According to Addiction Medicine Canada’s letter, the BC Centre on Substance Use posed “fundamental questions” to the B.C. government, potentially causing the delay.
“We’re stuck in a place where the government publicly has said it’s told BCCSU to make guidance, and BCCSU has said it’s waiting for government to tell them what to do,” Melamed told Canadian Affairs.
This lag has frustrated addiction specialists, who argue the lack of clear guidance is impeding the transition to witnessed dosing and jeopardizing patient care. They warn that permitting take-home drugs leads to more diversion onto the streets, putting individuals at greater risk.
“Diversion of prescribed alternatives expands the number of people using opioids, and dying from hydromorphone and fentanyl use,” reads the letter, which was also co-signed by Dr. Robert Cooper and Dr. Michael Lester. The doctors are founding board members of Addiction Medicine Canada, a nonprofit that advises on addiction medicine and advocates for research-based treatment options.
“We have had people come in [to our clinic] and say they’ve accessed hydromorphone on the street and now they would like us to continue [prescribing] it,” Melamed told Canadian Affairs.
A spokesperson for the BC Centre on Substance Use declined to comment, referring Canadian Affairs to the Ministry of Health. The ministry was unable to provide comment by the publication deadline.
Big challenges
Under the witnessed dosing model, doctors, nurses and pharmacists will oversee consumption of opioids such as hydromorphone, methadone and morphine in clinics or pharmacies.
The shift back to witnessed dosing will place significant demands on pharmacists and patients. In April 2024, an estimated 4,400 people participated in B.C.’s safer supply program.
Chris Chiew, vice president of pharmacy and health-care innovation at the pharmacy chain London Drugs, told Canadian Affairs that the chain’s pharmacists will supervise consumption in semi-private booths.
Nathan Wong, a B.C.-based pharmacist who left the profession in 2024, fears witnessed dosing will overwhelm already overburdened pharmacists, creating new barriers to care.
“One of the biggest challenges of the retail pharmacy model is that there is a tension between making commercial profit, and being able to spend the necessary time with the patient to do a good and thorough job,” he said.
“Pharmacists often feel rushed to check prescriptions, and may not have the time to perform detailed patient counselling.”
Others say the return to witnessed dosing could create serious challenges for individuals who do not live close to health-care providers.
Shelley Singer, a resident of Cowichan Bay, B.C., on Vancouver Island, says it was difficult to make multiple, daily visits to a pharmacy each day when her daughter was placed on witnessed dosing years ago.
“It was ridiculous,” said Singer, whose local pharmacy is a 15-minute drive from her home. As a retiree, she was able to drive her daughter to the pharmacy twice a day for her doses. But she worries about patients who do not have that kind of support.
“I don’t believe witnessed supply is the way to go,” said Singer, who credits safer supply with saving her daughter’s life.
Melamed notes that not all safer supply medications require witnessed dosing.
“Methadone is under witness dosing because you start low and go slow, and then it’s based on a contingency management program,” she said. “When the urine shows evidence of no other drug, when the person is stable, [they can] take it at home.”
She also noted that Suboxone, a daily medication that prevents opioid highs, reduces cravings and alleviates withdrawal, does not require strict supervision.
Kendra Wong, of the B.C. health ministry, told Canadian Affairs that long-acting medications such as methadone and buprenorphine could be reintroduced to help reduce the strain on health-care professionals and patients.
“There are medications available through the [safer supply] program that have to be taken less often than others — some as far apart as every two to three days,” said Wong.
“Clinicians may choose to transition patients to those medications so that they have to come in less regularly.”
Such an approach would align with Addiction Medicine Canada’s recommendations to the ministry.
The group says it supports supervised dosing of hydromorphone as a short-term solution to prevent diversion. But Melamed said the long-term goal of any addiction treatment program should be to reduce users’ reliance on opioids.
The group recommends combining safer supply hydromorphone with opioid agonist therapies. These therapies use controlled medications to reduce withdrawal symptoms, cravings and some of the risks associated with addiction.
They also recommend limiting unsupervised hydromorphone to a maximum of five 8 mg tablets a day — down from the 30 tablets currently permitted with take-home supplies. And they recommend that doses be tapered over time.
“This protocol is being used with success by clinicians in B.C. and elsewhere,” the letter says.
“Please ensure that the administrative delay of the implementation of your new policy is not used to continue to harm the public.”
This article was produced through the Breaking Needles Fellowship Program, which provided a grant to Canadian Affairs, a digital media outlet, to fund journalism exploring addiction and crime in Canada. Articles produced through the Fellowship are co-published by Break The Needle and Canadian Affairs.
Subscribe to Break The Needle
2025 Federal Election
Poilievre to invest in recovery, cut off federal funding for opioids and defund drug dens

From Conservative Party Communications
Poilievre will Make Recovery a Reality for 50,000 Canadians
Conservative Leader Pierre Poilievre pledged he will bring the hope that our vulnerable Canadians need by expanding drug recovery programs, creating 50,000 new opportunities for Canadians seeking freedom from addiction. At the same time, he will stop federal funding for opioids, defund federal drug dens, and ensure that any remaining sites do not operate within 500 meters of schools, daycares, playgrounds, parks and seniors’ homes, and comply with strict new oversight rules that focus on pathways to treatment.
More than 50,000 people have lost their lives to fentanyl since 2015—more Canadians than died in the Second World War. Poilievre pledged to open a path to recovery while cracking down on the radical Liberal experiment with free access to illegal drugs that has made the crisis worse and brought disorder to local communities.
Specifically, Poilievre will:
- Fund treatment for 50,000 Canadians. A new Conservative government will fund treatment for 50,000 Canadians in treatment centres with a proven record of success at getting people off drugs. This includes successful models like the Bruce Oake Recovery Centre, which helps people recover and reunite with their families, communities, and culture. To ensure the best outcomes, funding will follow results. Where spaces in good treatment programs exist, we will use them, and where they need to expand, these funds will allow that.
- Ban drug dens from being located within 500 metres of schools, daycares, playgrounds, parks, and seniors’ homes and impose strict new oversight rules. Poilievre also pledged to crack down on the Liberals’ reckless experiments with free access to illegal drugs that allow provinces to operate drug sites with no oversight, while pausing any new federal exemptions until evidence justifies they support recovery. Existing federal sites will be required to operate away from residential communities and places where families and children frequent and will now also have to focus on connecting users with treatment, meet stricter regulatory standards or be shut down. He will also end the exemption for fly-by-night provincially-regulated sites.
“After the Lost Liberal Decade, Canada’s addiction crisis has spiralled out of control,” said Poilievre. “Families have been torn apart while children have to witness open drug use and walk through dangerous encampments to get to school. Canadians deserve better than the endless Liberal cycle of crime, despair, and death.”
Since the Liberals were first elected in 2015, our once-safe communities have become sordid and disordered, while more and more Canadians have been lost to the dangerous drugs the Liberals have flooded into our streets. In British Columbia, where the Liberals decriminalized dangerous drugs like fentanyl and meth, drug overdose deaths increased by 200 percent.
The Liberals also pursued a radical experiment of taxpayer-funded hard drugs, which are often diverted and resold to children and other vulnerable Canadians. The Vancouver Police Department has said that roughly half of all hydromorphone seizures were diverted from this hard drugs program, while the Waterloo Regional Police Service and Niagara Regional Police Service said that hydromorphone seizures had exploded by 1,090% and 1,577%, respectively.
Despite the death and despair that is now common on our streets, bizarrely Mark Carney told a room of Liberal supporters that 50,000 fentanyl deaths in Canada is not “a crisis.” He also hand-picked a Liberal candidate who said the Liberals “would be smart to lean into drug decriminalization” and another who said “legalizing all drugs would be good for Canada.”
Carney’s star candidate Gregor Robertson, an early advocate of decriminalization and so-called safe supply, wanted drug dens imposed on communities without any consultation or public safety considerations. During his disastrous tenure as Vancouver Mayor, overdoses increased by 600%.
Alberta has pioneered an approach that offers real hope by adopting a recovery-focused model of care, leading to a nearly 40 percent reduction in drug-poisoning deaths since 2023—three times the decrease seen in British Columbia. However, we must also end the Liberal drug policies that have worsened the crisis and harmed countless lives and families.
To fund this policy, a Conservative government will stop federal funding for opioids, defund federal drug dens, and sue the opioid manufacturers and consulting companies who created this crisis in the first place.
“Canadians deserve better than the Liberal cycle of crime, despair, and death,” said Poilievre. “We will treat addiction with compassion and accountability—not with more taxpayer-funded poison. We will turn hurt into hope by shutting down drug dens, restoring order in our communities, funding real recovery, and bringing our loved ones home drug-free.”
-
 2025 Federal Election2 days ago
2025 Federal Election2 days agoOttawa Confirms China interfering with 2025 federal election: Beijing Seeks to Block Joe Tay’s Election
-

 2025 Federal Election1 day ago
2025 Federal Election1 day agoBREAKING: THE FEDERAL BRIEF THAT SHOULD SINK CARNEY
-

 COVID-192 days ago
COVID-192 days agoNearly Half of “COVID-19 Deaths” Were Not Due to COVID-19 – Scientific Reports Journal
-

 2025 Federal Election2 days ago
2025 Federal Election2 days agoHow Canada’s Mainstream Media Lost the Public Trust
-

 2025 Federal Election21 hours ago
2025 Federal Election21 hours agoMark Carney Wants You to Forget He Clearly Opposes the Development and Export of Canada’s Natural Resources
-
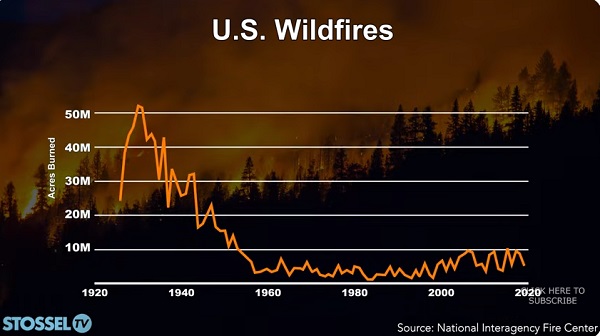
 John Stossel2 days ago
John Stossel2 days agoClimate Change Myths Part 2: Wildfires, Drought, Rising Sea Level, and Coral Reefs
-

 2025 Federal Election1 day ago
2025 Federal Election1 day agoCHINESE ELECTION THREAT WARNING: Conservative Candidate Joe Tay Paused Public Campaign
-

 International13 hours ago
International13 hours agoPope Francis’ body on display at the Vatican until Friday







