Addictions
“Government Heroin” documentary exposes rampant safer supply fraud

By Adam Zivo
There is no substitute for hearing testimony with your own ears and eyes.
Although there is ample evidence that Canada’s “safer supply” programs are being widely defrauded and flooding communities with opioids, advocates continue to deny that this problem exists. That’s why I premiered my new documentary this week, “Government Heroin,” which follows the story of Callum Bagnall, a 25-year-old student who purchased thousands of diverted safer supply pills in London, Ontario.
While many written accounts of safer supply fraud have been published in the Canadian media, this documentary provides, for the first time, an extended interview with a former addict who openly describes his own use of these diverted drugs. It is one thing to read these stories, and altogether another to watch and listen to them – so perhaps this will help dispel the myths that have been pushed, rather aggressively, by the harm reduction movement.
In the film, Callum explains how, three years ago, a friend informed him that drug users in the city were receiving “insane” amounts of free safer supply drugs – predominantly hydromorphone, an opioid as potent as heroin. While these drugs are meant to wean addicts off riskier street substances, the friend explained that recipients mostly sell their safer supply at bargain prices so they can procure stronger substances, such as illicit fentanyl.
At first, Callum thought this was a joke. He had been struggling with a moderate addiction to pharmaceutical opioids – mostly oxycodone and Percocet – but, as these pills were expensive and hard to find, his drug use remained stable. The idea that the government was showering individuals with hundreds of powerful opioid pills a month, for free and with essentially no supervision, seemed “almost like a dream for a drug addict.”
But then he connected with some safer supply clients and realized that everything that he had heard was true. Fueled by a near-limitless supply of dirt-cheap opioids, Callum’s drug use rapidly spun out of control and, for two years, his life fell into utter disarray. Although he went to rehab last year, he says that his mind remains muddled by the aftereffects of these drugs to this day.
“I would have already been at the end of my road and (would) have gone to rehab at that point, if safer supply drugs weren’t so cheap and available. With the small amount of money I was making, I was able to afford hundreds of safer supply pills a week because of how cheap they were,” he says.
It was obvious to Callum that these pills were not counterfeit, given their quality and consistency and the fact that they typically came in their original, labelled prescription bottles: “Usually the people I was buying them from would try to scratch out the doctor’s name or their name. They were kind of paranoid about that. But sometimes they would just give it to me with the label unripped, not covered with marker or anything.”
Callum estimates that 90 percent of the safer supply clients he interacted with were diverting their drugs – a figure that is fairly consistent with estimates provided by former drug users I interviewed in London last year, who typically placed the diversion rate among their circles at around 80 percent.
Callum also believes that organized crime is involved in the trafficking of these drugs, and recalled how one higher-level dealer said that he would drive to northern Ontario, where safer supply is essentially unavailable, with thousands of pills stowed in his trunk to resell at a significant profit.
Subscribe for free to get BTN’s latest news and analysis, or donate to our journalism fund.
While I was unable to independently verify Callum’s claim about intraprovincial trafficking, his testimony is consistent with information provided to me earlier this year by Michael Tibollo, Ontario’s Associate Minister of Mental Health and Addictions, who said that, based on certain police reports and epidemiological data, it is clear that there is a particular problem with safer supply drugs being trafficked from London to northern Ontario.
Callum was able to corroborate the general contours of his story by providing dozens of screenshots of time-stamped text conversations between himself and his former dealers (some of which appear in the documentary), as well as excerpts of his medical records indicating that he had been diagnosed with severe opioid use disorder and had been “buying safer supply from friends.”
He also called a safer supply patient whom he used to purchase drugs from, and, while I listened in, had her confirm that she had hundreds of pills ready to sell and could introduce him to a safer supply doctor if he wanted to get on the program. A video recording of this conversation was originally meant to be included in the documentary, but was cut to mitigate risk of retaliation.
Finally, Callum’s mother, a registered nurse, appears in the documentary and recounts finding safer supply prescription bottles in her son’s room on the day he went to rehab.
As public scrutiny of safer supply has increased over the past year, providers have insisted that they are closely monitoring diversion through urine testing. Yet Callum says that the clients he interacted with would occasionally, in the process of selling their drugs, withhold a few of their pills and openly admit to him that they needed these small amounts to pass their tests.
“(They) would also take one or two pills the night before they get their prescription, so that it looks like it’s in their system. It shows up on the urine tests. So they would use that to pass the urine tests, so that they would get another script the next week,” he says in the film.
The exploitation of this loophole was confirmed by Dr. Janel Gracey, an addiction physician who treated Callum and who is also featured in my documentary. She says that “it is known in the addiction world that urine testing is not effective at catching diversion” because such tests only measure the presence of a drug, not its quantity. A safer supply patient can divert almost all of their drugs and still pass their urine tests, she says, so long as they take just one pill before giving their samples.
Gracey characterizes Canada’s current safer supply system as an underregulated “free for all” that destabilizes patients while allowing some pharmacists and physicians to reap considerable profits. “I know people on the safer supply program that have never even used fentanyl, and that’s the whole point of the program: to get them off the fentanyl. So they’re just lining up and getting a bunch of (hydromorphone), really, for no reason,” she says.
Gracey estimates that, of her 400 patients, approximately half have used, or know someone who has used, diverted safer supply drugs. She says that inexpensive hydromorphone is now “readily available on every street corner here in London,” and that dealers are “bombarding” her patients with the drug, causing many of them to “fall off the rails.”
“We are seeing younger and younger patients come in, unfortunately. Fifteen (and) 16-year-olds coming in, and they’re getting hooked on (hydromorphone) because it’s so incredibly cheap. It’s cheaper than alcohol,” she says. “We do get a few coming in that are there because of fentanyl use, but usually even the (young fentanyl users) started with (hydromorphone).”
I encourage you to watch “Government Heroin,” as the 19-minute documentary provides a more visceral and comprehensive account of the harms described here. There is no substitute for hearing testimony with your own ears and eyes.
This article was originally published in The Bureau, a Canadian media outlet that investigates the intersections of organized crime, drug trafficking and foreign interference.
Subscribe to Break The Needle. Our content is always free – but if you want to help us commission more high-quality journalism, consider getting a voluntary paid subscription.
Addictions
Why B.C.’s new witnessed dosing guidelines are built to fail
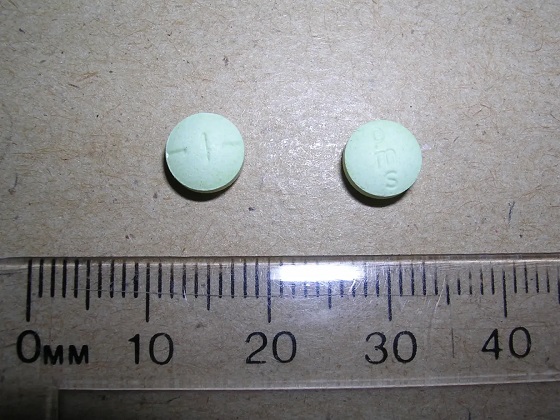
Photo by Acceptable at English Wikipedia, ‘Two 1 mg pills of Hydromorphone, prescribed to me after surgery.’ [Licensed under CC BY-SA 3.0, via Wikimedia Commons]
By Alexandra Keeler
B.C. released new witnessed dosing guidelines for safer supply opioids. Experts say they are vague, loose and toothless
This February, B.C pledged to reintroduce witnessed dosing to its controversial safer supply program.
Safer supply programs provide prescription opioids to people who use drugs. Witnessed dosing requires patients to consume those prescribed opioids under the supervision of a health-care professional, rather than taking their drugs offsite.
The province said it was reintroducing witnessed dosing to “prevent the diversion of prescribed opioids and hold bad actors accountable.”
But experts are saying the government’s interim guidelines, released April 29, are fundamentally flawed.
“These guidelines — just as any guidelines for safer supply — do not align with addiction medicine best practices, period,” said Dr. Leonara Regenstreif, a primary care physician specializing in substance use disorders. Regenstreif is a founding member of Addiction Medicine Canada, an advocacy group that represents 23 addiction specialists.
Addiction physician Dr. Michael Lester, who is also a founding member of the group, goes further.
“Tweaking a treatment protocol that should not have been implemented in the first place without prior adequate study is not much of an advancement,” he said.
Witnessed dosing
Initially, B.C.’s safer supply program was generally administered through witnessed dosing. But in 2020, to facilitate access amidst pandemic restrictions, the province moved to “take-home dosing,” allowing patients to take their prescription opioids offsite.
After pandemic restrictions were lifted, the province did not initially return to witnessed dosing. Rather, it did so only recently, after a bombshell government report alleged more than 60 B.C. pharmacies were boosting sales by encouraging patients to fill unnecessary opioid prescriptions. This incentivized patients to sell their medications on the black market.
B.C.’s interim guidelines, developed by the BC Centre on Substance Use at the government’s request, now require all new safer supply patients to begin with witnessed dosing.
But for existing patients, the guidelines say prescribers have discretion to determine whether to require witnessed dosing. The guidelines define an existing patient as someone who was dispensed prescription opioids within the past 30 days.
The guidelines say exemptions to witnessed dosing are permitted under “extraordinary circumstances,” where witnessed dosing could destabilize the patient or where a prescriber uses “best clinical judgment” and determines diversion risk is “very low.”
Holes
Clinicians say the guidelines are deliberately vague.
Regenstreif described them as “wordy, deliberately confusing.” They enable prescribers to carry on as before, she says.
Lester agrees. Prescribers would be in compliance with these guidelines even if “none of their patients are transferred to witnessed dosing,” he said.
In his view, the guidelines will fail to meet their goal of curbing diversion.
And without witnessed dosing, diversion is nearly impossible to detect. “A patient can take one dose a day and sell seven — and this would be impossible to detect through urine testing,” Lester said.
He also says the guidelines do not remove the incentive for patients to sell their drugs to others. He cites estimates from Addiction Medicine Canada that clients can earn up to $20,000 annually by selling part of their prescribed supply.
“[Prescribed safer supply] can function as a form of basic income — except that the community is being flooded with addictive and dangerous opioids,” Lester said.
Regenstreif warns that patients who had been diverting may now receive unnecessarily high doses. “Now you’re going to give people a high dose of opioids who don’t take opioids,” she said.
She also says the guidelines leave out important details on adjusting doses for patients who do shift from take-home to witnessed dosing.
“If a doctor followed [the guidelines] to the word, and the patient followed it to the word, the patient would go into withdrawal,” she said.
The guidelines assume patients will swallow their pills under supervision, but many crush and inject them instead, Regenstreif says. Because swallowing is less potent, a higher dose may be needed.
“None of that is accounted for in this document,” she said.
Survival strategy
Some harm reduction advocates oppose a return to witnessed dosing, saying it will deter people from accessing a regulated drug supply.
Some also view diversion as a life-saving practice.
Diversion is “a harm reduction practice rooted in mutual aid,” says a 2022 document developed by the National Safer Supply Community of Practice, a group of clinicians and harm reduction advocates.
The group supports take-home dosing as part of a broader strategy to improve access to safer supply medications. In their document, they say barriers to accessing safer supply programs necessitate diversion among people who use drugs — and that the benefits of diversion outweigh the risks.
However, the risks — and harms — of diversion are mounting.
People can quickly develop a tolerance to “safer” opioids and then transition to more dangerous substances. Some B.C. teenagers have said the prescription opioid Dilaudid was a stepping stone to them using fentanyl. In some cases, diversion of these drugs has led to fatal overdoses.
More recently, a Nanaimo man was sentenced to prison for running a highly organized drug operation that trafficked diverted safer supply opioids. He exchanged fentanyl and other illicit drugs for prescription pills obtained from participants in B.C.’s safer supply program.
Recovery
Lester, of Addiction Medicine Canada, believes clinical discretion has gone too far. He says take-home dosing should be eliminated.
“Best practices in addiction medicine assume physicians prescribing is based on sound and thorough research, and ensuring that their prescribing does not cause harm to the broader community, as well as the patient,” he said.
“[Safer supply] for opioids fails in both these regards.”
He also says safer supply should only be offered as a short-term bridge to patients being started on proven treatments like buprenorphine or methadone, which help reduce drug cravings and manage withdrawal symptoms.
B.C.’s witnessed dosing guidelines say prescribers can discuss such treatment options with patients. However, the guidelines remain neutral on whether safer supply is intended as a transitional step toward longer-term treatment.
Regenstreif says this neutrality undermines care.
“[M]ost patients I’ve seen with opioid use disorder don’t want to have [this disorder],” she said. “They would rather be able to set goals and do other things.”
Oversight gaps
Currently, about 3,900 people in B.C. participate in the safer supply program — down from 5,200 in March 2023.
The B.C. government has not provided data on how many have been transitioned to witnessed dosing. Investigative journalist Rob Shaw recently reported that these data do not exist.
“The government … confirmed recently they don’t have any mechanism to track which ‘safe supply’ participants are witnessed and which [are] not,” said Elenore Sturko, a Conservative MLA for Surrey-Cloverdale, who has been a vocal critic of safer supply.
“Without a public report and accountability there can be no confidence.”
The BC Centre on Substance Use, which developed the interim guidelines, says it does not oversee policy decisions or data tracking. It referred Canadian Affairs’ questions to B.C.’s Ministry of Health, which has yet to clarify whether it will track and publish transition data. The ministry did not respond to requests for comment by deadline.
B.C. has also not indicated when or whether it will release final guidelines.
Regenstreif says the flawed guidelines mean many people may be misinformed, discouraged or unsupported when trying to reduce their drug use and recover.
“We’re not listening to people with lived experience of recovery,” she said.
This article was produced through the Breaking Needles Fellowship Program, which provided a grant to Canadian Affairs, a digital media outlet, to fund journalism exploring addiction and crime in Canada. Articles produced through the Fellowship are co-published by Break The Needle and Canadian Affairs.
Subscribe to Break The Needle
Addictions
More young men want to restrict pornography: survey

From LifeSiteNews
Nearly 64% of American men now believe online pornography should be more difficult to access, with even higher numbers of women saying the same thing.
A new survey has shown that an increasing number of young men want more restrictions on online pornography.
According to a survey by the American Enterprise Institute’s Survey Center on American Life, nearly 7 in 10 (69 percent) of Americans support the idea of making online pornography less accessible. In 2013, 65 percent expressed support for policies restricting internet pornography.
The most substantial increase in the support for restrictive measures on pornography could be observed in young men (age 18-24). In 2013, about half of young men favored restrictions, while 40 percent actively opposed such policies. In 2025, 64 percent of men believe accessing online pornography should be made more difficult.
The largest support for restriction on internet pornography overall could be measured among older men (65+), where 73 percent favored restrictions. An even larger percentage of women in each age group supported making online pornography less accessible. Seventy-two percent of young women (age 18-24) favored restriction, while 87 percent of women 55 years or older expressed support for less accessibility of internet pornography.
Viewing pornography is highly addictive and can lead to serious health problems. Studies have shown that children often have their first encounter with pornography at around 12 years old, with boys having a lower average age of about 10-11, and some encountering online pornography as young as 8. Studies have also shown that viewing pornography regularly rewires humans brains and that children, adolescents, and younger men are especially at risk for becoming addicted to online pornography.
According to Gary Wilson’s landmark book on the matter, “Your Brain on Porn,” pornography addiction frequently leads to problems like destruction of genuine intimate relationships, difficulty forming and maintaining real bonds in relationship, depression, social anxiety, as well as reduction of gray matter, leading to desensitization and diminished pleasure from everyday activities among many others.
-

 illegal immigration2 days ago
illegal immigration2 days agoICE raids California pot farm, uncovers illegal aliens and child labor
-

 Uncategorized14 hours ago
Uncategorized14 hours agoCNN’s Shock Climate Polling Data Reinforces Trump’s Energy Agenda
-

 Business1 day ago
Business1 day agoTrump to impose 30% tariff on EU, Mexico
-

 Energy1 day ago
Energy1 day agoLNG Export Marks Beginning Of Canadian Energy Independence
-

 Business1 day ago
Business1 day agoCarney government should apply lessons from 1990s in spending review
-

 Entertainment1 day ago
Entertainment1 day agoStudy finds 99% of late-night TV guests in 2025 have been liberal
-

 Frontier Centre for Public Policy14 hours ago
Frontier Centre for Public Policy14 hours agoCanada’s New Border Bill Spies On You, Not The Bad Guys
-

 Opinion7 hours ago
Opinion7 hours agoPreston Manning: Three Wise Men from the East, Again








