Addictions
B.C. poll reveals clash between Indigenous views and drug policy


By Alexandra Keeler
A supermajority of First Nations respondents disagree that criminalizing drug use is racist, challenging public health advocates’ assumptions
A new report shows a majority of British Columbians — and a plurality of all ethnic communities surveyed — disagree with the contention that drug criminalization policies are racist.
The findings challenge assertions made by prominent B.C. policymakers, who have advocated for drug decriminalization and harm-reduction initiatives on the grounds of anti-racism and reconciliation.
The report, published by the policy nonprofit Centre for Responsible Drug Policy and think tank Macdonald-Laurier Institute, draws from a poll of 6,300 B.C. adults that was commissioned by the centre and conducted by Mainstreet Research.
“Chinese and Indigenous leaders keep telling me that their communities are very anti-drug, but public health officials and harm-reduction activists keep saying that legalization is integral to anti-racism and reconciliation,” said Adam Zivo, a journalist and founder of the centre.
“Now we have data to show which side is more accurate.”
When asked whether criminalizing drug use is racist, just 22 per cent of all respondents agreed, while 60 per cent disagreed. Notably, 79 percent of the respondents identified as white.
Disagreement was strongest among First Nations respondents, with just nine per cent of the 172 Indigenous respondents agreeing that criminalization is racist and 67 per cent disagreeing.
Agreement was stronger among Asian communities, with East Asian and South Asian respondents being most likely to say criminalization policies are racist.
In the East Asian cohort, 42 per cent said they disagreed that criminalizing drug use is racist, while 36 per cent strongly agreed. Similarly, 46 per cent of South Asian respondents disagreed and 32 per cent agreed.
Self-determination
The poll challenges views articulated by some prominent B.C. policymakers and public health groups.
In July, B.C.’s provincial health officer, Dr. Bonnie Henry, released a report asserting that drug policies prohibiting the use of hard drugs are rooted in racism and colonialism.
“Prohibitionist drug policies are deeply rooted in colonialism, reflecting and perpetuating systemic racism that disproportionately impacts Indigenous peoples,” Henry’s report says.
“These policies were designed to control marginalized populations and have led to over-incarceration, intergenerational trauma, and significant health disparities within these communities.”
Henry’s report contends that decriminalization policies — such as those implemented by B.C. as part of a three-year trial project that began January 2023 — can help to rectify these injustices by prioritizing health and safety over law enforcement.
Henry’s report was released mere months after B.C. rolled back some of its decriminalization measures in response to growing public concerns over decriminalization’s effects on community safety and order. Henry’s report, which is published by the BC Ministry of Health, urges the province to move in the opposite direction.
“This report’s recommendation is to continue to refine and expand prescribed alternatives to unregulated drugs, and critically, to explore implementation of models that do not require prescription,” Henry writes, referring to harm-reduction initiatives such as safer supply that dispense prescription opioids to drug users.
The report presents decriminalization as a move supported by Indigenous communities, citing the Declaration on the Rights of Indigenous Peoples Act Action Plan. Action 4.12 aims to “address the disproportionate impacts of the overdose public health emergency on Indigenous Peoples by: applying to the Government of Canada to decriminalize simple possession of small amounts of illicit drugs for personal use.”
The Canadian Drug Policy Coalition, a policy advocacy group based out of Simon Fraser University, has similarly contended that drug criminalization is racist.
The coalition’s website says, “the demand by Black communities to decriminalize drugs and to immediately expunge records are a vital necessity for minimizing the racially disproportionate harms of drug criminalization, part of a broader struggle to end the war on Black communities.”
And in December 2023, the Harm Reduction Nurses Association, a national organization that advances harm-reduction nursing, obtained an injunction to prevent the B.C. government from imposing restrictions on public drug consumption.
The association alleged the government’s actions “would put people at greater risk of fatal overdose, make healthcare outreach more challenging, and drive racial discrimination, particularly against Indigenous people.”
Subscribe for free to get BTN’s latest news and analysis, or donate to our journalism fund.
Minority polling challenges
Some Indigenous groups have expressed reservations about blanket decriminalization policies in other contexts.
In January 2024, the First Nations Health Authority, an agency that manages health services for Indigenous communities in B.C., issued a statement acknowledging decriminalization may not be the best approach for all communities.
“FNHA acknowledges and supports the self-determination of each First Nations community when considering implementing this exemption,” the statement reads, referring to the three-year exemption B.C. obtained from federal laws prohibiting the use of hard drugs.
First Nations Health Authority has emphasized the need for culturally informed approaches that prioritize community health and safety and advocated for nuanced strategies tailored to each community’s specific needs.
The Mainstreet Research poll reveals challenges in accurately representing the views of B.C.’s smaller ethnic communities.
While non-white Canadians make up 40 per cent of B.C.’s population, they accounted for only 16 per cent of the poll’s 6,300 respondents.
Responses by Black, Middle Eastern and Southeast Asian respondents were excluded from the current analysis because sample sizes were too small, numbering below 100. The English-only and automated telephone polling format may also increase uncertainty.
As the poll focused primarily on B.C. and broad drug policy questions, its findings underscore the need for a deeper understanding of community beliefs to inform drug policies.
The Centre for Responsible Drug Policy is releasing the polling data and its report on a “preliminary” basis so it can inform drug policy discussions ahead of provincial elections, which are taking place this October in B.C., Saskatchewan and New Brunswick.
But Mainstreet Research is continuing to gather data, aiming for a final survey size of more than 12,000 respondents. Once completed, the survey will be one of the largest polls on harm reduction ever conducted in Canada.
“The final report, set to be released later this year, will include larger samples from B.C.’s diverse ethnic communities, providing further clarity on their beliefs,” Zivo said.
This article was produced through the Breaking Needles Fellowship Program, which provided a grant to Canadian Affairs, a digital media outlet, to fund journalism exploring addiction and crime in Canada. Articles produced through the Fellowship are co-published by Break The Needle and Canadian Affairs.
Subscribe to Break The Needle. Our content is always free – but if you want to help us commission more high-quality journalism, consider getting a voluntary paid subscription.
Addictions
Four new studies show link between heavy cannabis use, serious health risks

Cannabis products purchased in Ontario and B.C., including gummies, pre-rolled joints, chocolates and dried flower; April 11, 2025. [Photo credit: Alexandra Keeler]
By Alexandra Keeler
New Canadian research shows a connection between heavy cannabis use and dementia, heart attacks, schizophrenia and even death
Six months ago, doctors in Boston began noticing a concerning trend: young patients were showing up in emergency rooms with atypical symptoms and being diagnosed with heart attacks.
“The link between them was that they were heavy cannabis users,” Dr. Ahmed Mahmoud, a cardiovascular researcher and physician in Boston, told Canadian Affairs in an interview.
These frontline observations mirror emerging evidence by Canadian researchers showing heavy cannabis use is associated with significant adverse health impacts, including heart attacks, schizophrenia and dementia.
Sources warn public health measures are not keeping pace with rapid changes to cannabis products as the market is commercialized.
“The irony of this moment is that society’s risk perception of cannabis is at an all-time low, at the exact moment that the substance is probably having increasingly negative health impacts,” said Dr. Daniel Myran, a physician and Canada Research Chair at the University of Ottawa. Myran was lead researcher on three new Canadian studies on cannabis’ negative health impacts.
Legalization
Canada was the first G7 country to create a commercial cannabis market when it legalized the production and sale of cannabis in 2018.
The drug is now widely used in Canada.
In the 2024 Canadian Cannabis Survey, an annual government survey of cannabis trends, 26 per cent of respondents said they used cannabis for non-medical purposes in the past year, up from 22 per cent in 2018. Among youth, that number was 41 per cent.
Health Canada’s website warns that cannabis use can lower blood pressure and raise heart rates, which can increase the risk of a heart attack. But the warnings on cannabis product labels vary. Some mention risks of anxiety or effects on memory and concentration, but make no mention of cardiovascular risks.
The annual cannabis survey also shows a significant percentage of Canadians remain unaware of cannabis’ health risks.
In the survey, only 70 per cent of respondents said they had enough reliable information to make informed decisions about cannabis use. And 50 per cent of respondents said they had not seen any education campaigns or public health messages about cannabis.
At the same time, researchers are finding mounting evidence that cannabis use is associated with health risks.
A 2023 study by researchers at the University of Calgary, the University of Alberta and Alberta Health Services found that adults with cannabis use disorder faced a 60 per cent higher risk of experiencing adverse cardiovascular events — including heart attacks. Cannabis use disorder is marked by the inability to stop using cannabis despite negative consequences, such as work, social, legal or health issues.
Between February and April of this year, three other Canadian studies linked frequent cannabis use to elevated risks of developing schizophrenia, dementia and mortality. These studies were primarily conducted by researchers at the Ottawa Hospital Research Institute and ICES uOttawa (formerly the Institute for Clinical Evaluative Sciences).
“These results suggest that individuals who require hospital-based care for a [cannabis use disorder] may be at increased risk of premature death,” said the study linking cannabis-related hospital visits with increased mortality rates.
The three 2024 studies all examined the impacts of severe cannabis use, suggesting more moderate users may face lower risks. The researchers also cautioned that their research shows a correlation between heavy cannabis use and adverse health effects, but does not establish causality.
Subscribe for free to get BTN’s latest news and analysis – or donate to our investigative journalism fund.
Budtenders
Health experts say they are troubled by the widespread perception that cannabis is entirely benign.
“It has some benefits, it has some side effects,” said Mahmoud, the Boston cardiovascular researcher. “We need to raise awareness about the side effects as well as the benefits.”
Some also expressed concern that the commercialization of cannabis products in Canada has created a race to produce products with elevated levels of THC, the main psychoactive compound that produces a “high.”
THC levels have more than doubled since legalization, yet even products with high THC levels are marketed as harmless.
“The products that are on the market are evolving in ways that are concerning,” Myran said. “Higher THC products are associated with considerably more risk.”
Myran views cannabis decriminalization as a public health success, because it keeps young people out of the criminal justice system and reduces inequities faced by Indigenous and racialized groups.
“[But] I do not think that you need to create a commercial cannabis market or industry in order to achieve those public health benefits,” he said.
Since decriminalization, the provinces have taken different approaches to regulating cannabis. But even in provinces where governments control cannabis distribution, such as New Brunswick and Nova Scotia, products with high THC levels dominate retail shelves and online storefronts.
In Myran’s view, federal and provincial governments should instead be focused on curbing harmful use patterns, rather than promoting cannabis sales.
Ian Culbert, executive director of the Canadian Public Health Association, thinks governments’ financial interest in the cannabis industry creates a conflict of interest.
“[As with] all regulated substances, governments are addicted to the revenue they create,” he said. “But they also have a responsibility to safeguard the well-being of citizens.”
Culbert believes cannabis retailers should be required to educate customers about health risks — just as bartenders are required to undergo Smart Serve training and lottery corporations are required to mitigate risks of gambling addiction.
“Give ‘budtenders’ the training around potential health risks,” he said.
“While cannabis may not be the cause of some of these negative health events … it is the intersection at which an intervention can take place through the transaction of sales. So is there something we can do there that can change the trajectory of a person’s life?”
This article was produced through the Breaking Needles Fellowship Program, which provided a grant to Canadian Affairs, a digital media outlet, to fund journalism exploring addiction and crime in Canada. Articles produced through the Fellowship are co-published by Break The Needle and Canadian Affairs.
Our content is always free – but if you want to help us commission more high-quality journalism, consider getting a voluntary paid subscription.
2025 Federal Election
Study links B.C.’s drug policies to more overdoses, but researchers urge caution

By Alexandra Keeler
A study links B.C.’s safer supply and decriminalization to more opioid hospitalizations, but experts note its limitations
A new study says B.C.’s safer supply and decriminalization policies may have failed to reduce overdoses. Furthermore, the very policies designed to help drug users may have actually increased hospitalizations.
“Neither the safer opioid supply policy nor the decriminalization of drug possession appeared to mitigate the opioid crisis, and both were associated with an increase in opioid overdose hospitalizations,” the study says.
The study has sparked debate, with some pointing to it as proof that B.C.’s drug policies failed. Others have questioned the study’s methodology and conclusions.
“The question we want to know the answer to [but cannot] is how many opioid hospitalizations would have occurred had the policy not have been implemented,” said Michael Wallace, a biostatistician and associate professor at the University of Waterloo.
“We can never come up with truly definitive conclusions in cases such as this, no matter what data we have, short of being able to magically duplicate B.C.”
Jumping to conclusions
B.C.’s controversial safer supply policies provide drug users with prescription opioids as an alternative to toxic street drugs. Its decriminalization policy permitted drug users to possess otherwise illegal substances for personal use.
The peer-reviewed study was led by health economist Hai Nguyen and conducted by researchers from Memorial University in Newfoundland, the University of Manitoba and Weill Cornell Medicine, a medical school in New York City. It was published in the medical journal JAMA Health Forum on March 21.
The researchers used a statistical method to create a “synthetic” comparison group, since there is no ideal control group. The researchers then compared B.C. to other provinces to assess the impact of certain drug policies.
Examining data from 2016 to 2023, the study links B.C.’s safer supply policies to a 33 per cent rise in opioid hospitalizations.
The study says the province’s decriminalization policies further drove up hospitalizations by 58 per cent.
“Neither the safer supply policy nor the subsequent decriminalization of drug possession appeared to alleviate the opioid crisis,” the study concludes. “Instead, both were associated with an increase in opioid overdose hospitalizations.”
The B.C. government rolled back decriminalization in April 2024 in response to widespread concerns over public drug use. This February, the province also officially acknowledged that diversion of safer supply drugs does occur.
The study did not conclusively determine whether the increase in hospital visits was due to diverted safer supply opioids, the toxic illicit supply, or other factors.
“There was insufficient evidence to conclusively attribute an increase in opioid overdose deaths to these policy changes,” the study says.
Nguyen’s team had published an earlier, 2024 study in JAMA Internal Medicine that also linked safer supply to increased hospitalizations. However, it failed to control for key confounders such as employment rates and naloxone access. Their 2025 study better accounts for these variables using the synthetic comparison group method.
The study’s authors did not respond to Canadian Affairs’ requests for comment.
Subscribe for free to get BTN’s latest news and analysis – or donate to our investigative journalism fund.
Correlation vs. causation
Chris Perlman, a health data and addiction expert at the University of Waterloo, says more studies are needed.
He believes the findings are weak, as they show correlation but not causation.
“The study provides a small signal that the rates of hospitalization have changed, but I wouldn’t conclude that it can be solely attributed to the safer supply and decrim[inalization] policy decisions,” said Perlman.
He also noted the rise in hospitalizations doesn’t necessarily mean more overdoses. Rather, more people may be reaching hospitals in time for treatment.
“Given that the [overdose] rate may have gone down, I wonder if we’re simply seeing an effect where more persons survive an overdose and actually receive treatment in hospital where they would have died in the pre-policy time period,” he said.
The Nguyen study acknowledges this possibility.
“The observed increase in opioid hospitalizations, without a corresponding increase in opioid deaths, may reflect greater willingness to seek medical assistance because decriminalization could reduce the stigma associated with drug use,” it says.
“However, it is also possible that reduced stigma and removal of criminal penalties facilitated the diversion of safer opioids, contributing to increased hospitalizations.”
Karen Urbanoski, an associate professor in the Public Health and Social Policy department at the University of Victoria, is more critical.
“The [study’s] findings do not warrant the conclusion that these policies are causally associated with increased hospitalization or overdose,” said Urbanoski, who also holds the Canada Research Chair in Substance Use, Addictions and Health Services.
Her team published a study in November 2023 that measured safer supply’s impact on mortality and acute care visits. It found safer supply opioids did reduce overdose deaths.
Critics, however, raised concerns that her study misrepresented its underlying data and showed no statistically significant reduction in deaths after accounting for confounding factors.
The Nguyen study differs from Urbanoski’s. While Urbanoski’s team focused on individual-level outcomes, the Nguyen study analyzed broader, population-level effects, including diversion.
Wallace, the biostatistician, agrees more individual-level data could strengthen analysis, but does not believe it undermines the study’s conclusions. Wallace thinks the researchers did their best with the available data they had.
“We do not have a ‘copy’ of B.C. where the policies weren’t implemented to compare with,” said Wallace.
B.C.’s overdose rate of 775 per 100,000 is well above the national average of 533.
Elenore Sturko, a Conservative MLA for Surrey-Cloverdale, has been a vocal critic of B.C.’s decriminalization and safer supply policies.
“If the government doesn’t want to believe this study, well then I invite them to do a similar study,” she told reporters on March 27.
“Show us the evidence that they have failed to show us since 2020,” she added, referring to the year B.C. implemented safer supply.
This article was produced through the Breaking Needles Fellowship Program, which provided a grant to Canadian Affairs, a digital media outlet, to fund journalism exploring addiction and crime in Canada. Articles produced through the Fellowship are co-published by Break The Needle and Canadian Affairs.
Our content is always free – but if you want to help us commission more high-quality journalism,
consider getting a voluntary paid subscription.
-

 Alberta2 days ago
Alberta2 days agoLow oil prices could have big consequences for Alberta’s finances
-

 International2 days ago
International2 days agoHistory in the making? Trump, Zelensky hold meeting about Ukraine war in Vatican ahead of Francis’ funeral
-
 Business2 days ago
Business2 days agoIt Took Trump To Get Canada Serious About Free Trade With Itself
-

 C2C Journal2 days ago
C2C Journal2 days ago“Freedom of Expression Should Win Every Time”: In Conversation with Freedom Convoy Trial Lawyer Lawrence Greenspon
-

 2025 Federal Election1 day ago
2025 Federal Election1 day agoColumnist warns Carney Liberals will consider a home equity tax on primary residences
-

 2025 Federal Election23 hours ago
2025 Federal Election23 hours agoMark Carney: Our Number-One Alberta Separatist
-

 Opinion2 days ago
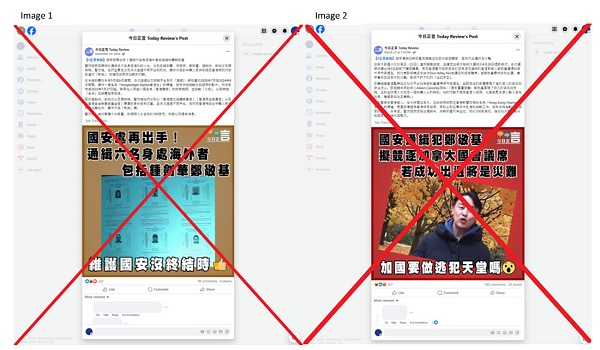
Opinion2 days agoCanadians Must Turn Out in Historic Numbers—Following Taiwan’s Example to Defeat PRC Election Interference
-

 International1 day ago
International1 day agoJeffrey Epstein accuser Virginia Giuffre reportedly dies by suicide